Related news by tag SELF-ASSEMBLY
Aspargi, Inbiomed, and nanoGUNE working hand in hand against Parkinson Disease
In 2014, Aspargi decided to financially contribute to the research on Parkinson Disease (PD) with the objective of increasing public awareness of both the disease and the need to investigate about its causes and treatments. The association started a fundraising campaign and opened a call for projects just after the 2014 Parkinson's World Day, 11th April. Because the idea was to promote collaboration, the projects were required to involve at least two different centers in Gipuzkoa.
In March 2015, the association announced that the winner of the 6 000€ award was an Inbiomed-nanoGUNE research project, led by Dr. Rosario Sánchez Pernaute, from Fundación Inbiomed, and Dr. Amaia Rebollo and Ikerbasque Research Professor Dr. Alexander Bittner, from nanoGUNE. This joint research project aims at developing better ways to grow neurons that could be used both to investigate and treat the disease.
The joint research project was initiated in 2012, when the researchers started thinking about new ways to implement the growth and the transplantation of neurons derived from stem cells, by using nanomaterials. “The aim of our research is to grow the cells in an environment similar to our brain. Usually, cells are treated and incubated in Petri dishes in the laboratories, but the results are not perfect”, Sánchez explains. "We believe this may happen (at least partly) because they are not grown in their natural environment, so we are working to recreate more natural conditions”, she adds.
At nanoGUNE, the researchers create a “nanospace”, made by a polymer fiber matrix, where cells automatically find a good place to fit. "We use a technique called electrospinning that allows to draw very fine fibers from a liquid polymer solution. We modify the polymer with the appropriate proteins, creating an environment similar to the natural environment that the neurons have in our brain”, explains Alexander Bittner, leader of the Self Assembly group at nanoGUNE. At Inbiomed, researchers grow the cells in fiber matrix, in order to obtain neurons that will behave like normal neurons. This allows investigating how the neurons grow, behave, and age.
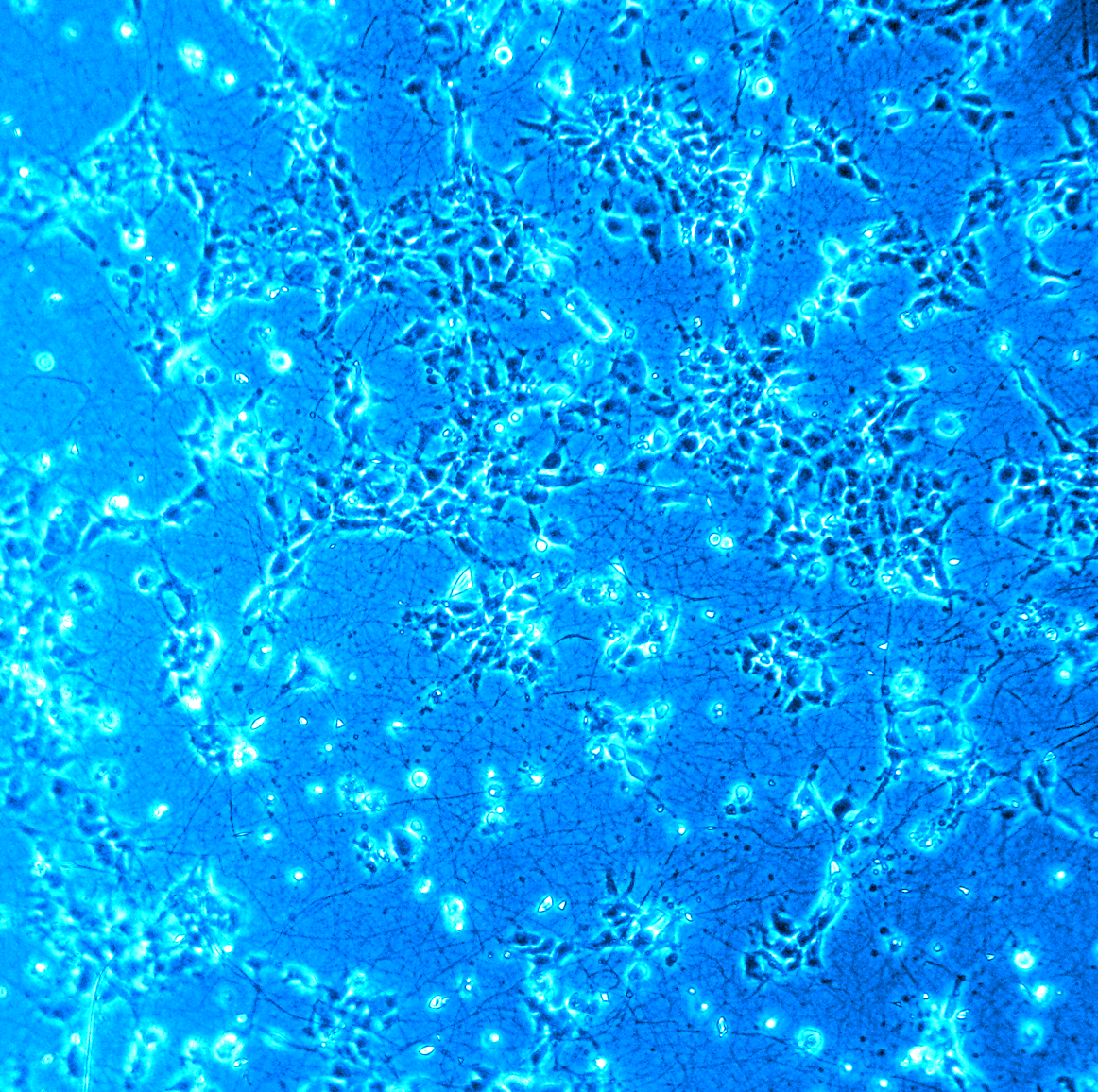
Towards a replacement therapy to treat Parkinson
Rosario Sánchez explains that Parkinson should be called a syndrome instead of disease, as it is a collection of symptoms that may have different causes. “Although there seem to be different causes for Parkinson, a common link is the loss of dopamine that occurs because the neurons producing it degenerate and die. Treatments nowadays consist in replacing dopamine by different means (drugs, cells, or genes) in order to improve the typical symptoms of Parkinson: tremor, slowness, difficulty in switching motor programs, etc.", Sánchez adds.
“New ideas for treating and preventing diseases do not always require drugs. In PD it is possible to replace damaged cells by new neurons”, explained Bittner. “The problem is that we need fresh cells for this; stem cells are in a very early developing stage, so that we can program them to grow and develop into the cell type that we need”, added Bittner. This “reprogramming” allows the use of stem cells, e.g. from the skin of the patient.
Replacement therapies to treat Parkinson are already being used at an experimental stage. This therapy could be an alternative to the use of pills with dopamine-based drugs that present two main problems: the loss of efficacy with time and the difficulty of knowing how much dopamine does the patient need. "Using cells, the amount of dopamine would be regulated internally, as they have the sensors, the (dopamine) receptors for that", Sánchez explains. "However ---she adds– one of the main problems for the classical replacement therapy is to obtain a sufficient amount of cells for the treatment, as these cells have to be obtained from a fetus in a very early stage of development". This is the reason why it is so important to find ways to obtain good functional neurons from stem cells (from the patient) for replacement therapies.
NanoReMedi, an innovative research project on regenerative medicine
Repair or replacement of tissue and organ functions, lost due to age, disease or damage, represents one of the most urgent medical needs of our aging society. The NanoReMedi consortium will contribute to addressing this fundamentally important issue by using a new and efficient scientific approach, relying on the design, preparation, characterization and validation of peptide-based functional nanomaterials.

